Skip NavigationSkip to Primary Content

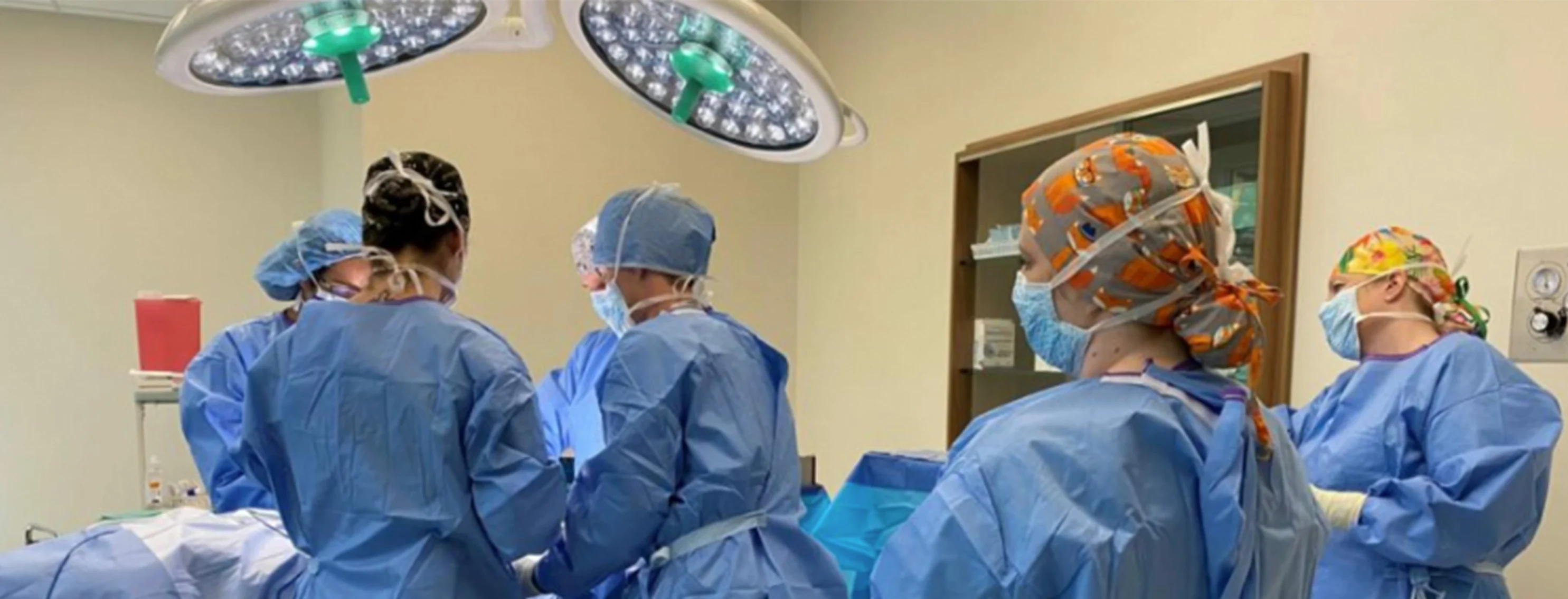


Services
At VetMED, our focus is thorough and comprehensive care for your pet.

Payment Options
For your convenience, we accept most payment methods.

rDVM Portal
Are you a veterinarian looking to submit a referral?

Careers at VetMED
Interested in learning more about career opportunities at VetMED?

VetMED Paw it Forward Fund
Help us, help animals

Pharmacy
Order food and medicine!
Client Testimonials & Reviews
We value our clients’ experience at VetMED Emergency & Specialty Veterinary Hospital. Here’s what some of your neighbors are saying about us.
Amazing staff and great care. What I appreciated most was everyone cared about the well-being of myself and my dog (Lady). They worked with me to get the best care for Lady while I got my injury seen too. They really helped make a traumatic experience easier. I cannot thank them enough!
Morgan B.
Amazing staff, quick wait times, quality service, and excellent communication. Jenna had a bee sting and her head swelled up the staff made us comfy and fixed her all up! Thank you! Will definitely be back for any future emergencies.
Lori B.
My puppy had an allergic reaction and I got a hold of that Med they were very helpful on getting started on treatment prior to my arrival to the office. The office front desk the vet techs and the veterinarian were extremely helpful and everyone was very kind. I would recommend them to anybody.
Cathy R.

